An Interview with Cryobiology Expert Dr. Jason Acker
Freezing is stressful for mammalian cells – to say the least. Cells face potentially dangerous ice crystals and severe dehydration when cooled to very low temperatures. Yet, by carefully configuring a cryopreservation protocol, cells can be shielded from injury. Thanks to discoveries in cryobiology, scientists have preserved many cell types to date, but further work is needed to safeguard the next generations of cell-based therapies. Storing and shipping cell therapy products usually requires cryopreservation. If the cells are damaged at the end of the process, patients may not only receive a less effective treatment but also face adverse effects.
We interviewed Jason Acker, Ph.D., to discuss the past, present, and future of cryobiology and its applications to medicine, including cell and gene therapies. Dr. Acker has over 25 years of experience studying how natural systems respond to environmental stress and adapting those strategies to preserve mammalian cells, tissues, and organs. He holds concurrent positions in research, applied science, and business: Professor in the Department of Medicine and Pathology at the University of Alberta, Senior Research Scientist with Canadian Blood Services, and Founder & CEO of PanTHERA CryoSolutions.
How did you get into cryobiology?
Dr. Jason Acker: I came from a small town in Alberta and went to an open house at the University of Alberta. There, I had an opportunity to go around and listen to a variety of professors talk about their research. One of them talked about frogs that can freeze and the biochemistry behind hibernation and cold tolerance. I thought that was fascinating, but it really didn’t click until later that semester. I was looking for a summer internship and serendipitously bumped into Professor Locksley McGann, whom I’d known for decades because he was a neighbor of my family’s, but I really didn’t know what he did. He told me about the field of cryobiology, and I was fascinated. I started working in his lab as a first-year undergraduate student and never looked back.
I completed my undergraduate degree and immediately did a master’s degree with Locksley as my supervisor. My master’s degree was starting to broach the idea of how ice forms within cells and complex tissues. I realized that one of, if not the best, cryobiology research groups in the world was in Edmonton, so I stayed on and did a Ph.D. Afterward, I did my postdoctoral fellowship at Harvard Medical School with Dr. Mehmet Toner and his team with the Center for Engineering in Medicine. That was an eye-opening experience and introduced me to the commercial opportunities with cryopreservation technology and a whole bunch of really, really neat science. We’ve stayed close collaborators since I left his group over 20 years ago.
Why is freezing cells so tricky?
JA: One of the challenges with freezing anything is the ice that forms. The damage that results from it is the biggest barrier to successful cryopreservation. And it’s the reason why we add cryoprotectants like dimethyl sulfoxide and glycerol to many of the solutions that we use to cryopreserve cells and tissues.
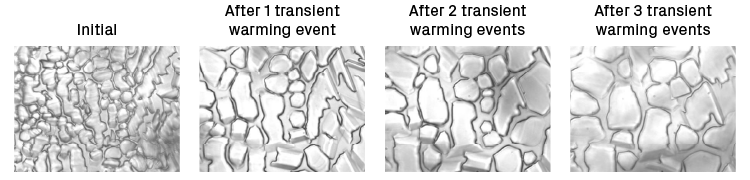
But the challenge is not necessarily the ice — and actually, this stems from early work I did as a master’s student and into my Ph.D. We showed in our early research that if you kept the ice crystals small, particularly those inside cells, they don’t do much damage. This was an observation that we built off of legacy work by a number of other scientists, including Peter Mazur, who is the “godfather of cryobiology”. And it’s the process of small ice crystals growing into large ice crystals that really is the damaging event, and that’s called ice recrystallization.
When Rob Ben and his team at Ottawa were exploring native antifreeze proteins, they realized that antifreeze proteins are hard to synthesize and are not very effective across the range of temperatures we need to use in cryobiology. But he leveraged his experience as an organic chemist to synthesize small versions of those antifreeze proteins that are very effective and potent ice recrystallization inhibitors. The exact mechanism is not well understood. What we do understand is that they likely interfere with the water structures around a growing ice crystal and make it very difficult for a liquid water molecule to join the frozen lattice. Because of that, it inhibits the ice crystal from growing from small to large.

It’s surprising that natural antifreeze proteins aren’t very effective. Why is that?
JA: If you look at the organisms — the fish, the insects — that survive freezing, they really don’t have to survive at very low temperatures. The fish, for example, live in salt water where the freezing point is only a couple of degrees below zero. As a result, preventing ice nucleation is a more effective strategy. If the ice does nucleate, the effectiveness of an ice recrystallization inhibitor doesn’t have to be as strong as what we’re using now to cryopreserve down to liquid nitrogen temperatures.
If the fish evolved over a glacial period where the temperatures were much colder, then they would have different antifreeze protein molecules. In fact, many of the terrestrial organisms, like insects, that do produce these have clearly evolved more potent antifreeze proteins, perhaps because of the environmental stress and the requirement to survive a larger temperature difference than what the fish had to.
Let’s shift to another area of your research – transient warming. What have you and others learned?
JA: We’ve known about transient warming for as long as we’ve been cryopreserving cells for therapeutic use — since early work with hematopoietic stem cells in the mid to late 80s. We recognized that the transient cycling of temperature was not good. When samples were being moved from liquid nitrogen storage to the clinic, we observed that you had to do this fast. We believed ice recrystallization was occurring, but from a practical perspective, there was not much that could be done. The impact of the transient warming wasn’t fully appreciated.
As cryobiologists — myself, Erik Woods, Allison Hubel, and several others who have been in the cell therapy industry for a while now — we’ve been cautioning that it’s not just the temperature of storage; it’s the cycling that we have to be concerned about. Some earlier studies, particularly with cord blood, suggested that transient warming was detrimental. Then we started to look at it from a data perspective. The first modern data set that came out was work we did with Dr. Nic Pineault and other scientists at Canadian Blood Services, where we intentionally induced transient warming in cord blood products and demonstrated the loss of potency and function of that product in a very controlled way. That paper came out a few years ago in Cytotherapy.
We know that transient warming occurs quickly, so the samples will thaw or warm faster than we think, particularly if they’re in small cryovials. Even full units of red cells will start to hit what we define as critical temperatures within minutes. It’s not tens of minutes; it’s minutes that you have to be worried about. Because of transient warming, handling becomes very important. People don’t understand the damage that they’re potentially doing to a product by simply taking it out of the freezer and putting it on the counter while they fill out some paperwork. You’re significantly damaging the samples. And we know that now.
“People don’t understand the damage that they’re potentially doing to a product by simply taking it out of the freezer and putting it on the counter while they fill out some paperwork. You’re significantly damaging the samples. And we know that now.”
What transient warming data is still needed?
JA: From my Canadian Blood Services perspective, I often got brought into conversations with our quality and operations folks when a freezer failed over the weekend, or there was a temperature excursion on a freezer that potentially exposed the products to a temperature above -65°C, which is the temperature written into regulations for the storage of red cells. I was often asked, what’s the impact? Can we use these products? The absence of data makes it nearly impossible to save those products because we need an evidence base.
We’ve undertaken a large multi-year project to collect data on red cells, specifically to show the impact of transient warming on products. That data set is incredibly comprehensive and is going to be the data set that hopefully serves the transfusion industry for decades from now. No one will want to repeat what we did in terms of the number of cycles, the range of cycles, and the scope and scale of the evaluation that we did.
But that’s the kind of data that we were missing. Now that the data is starting to come together, people are appreciating transient warming, and they’re looking for technologies or approaches that help mitigate that.
How can we mitigate the effects of transient warming for cryopreserved materials?
JA: Obviously, temperature control is so important. Technologies and strategies throughout the supply chain are critical to mitigate the transient warming that has significant detrimental effects on the quality of cell and gene therapy products. Azenta really understands that in terms of maintaining the cold chain throughout the handling of those products.
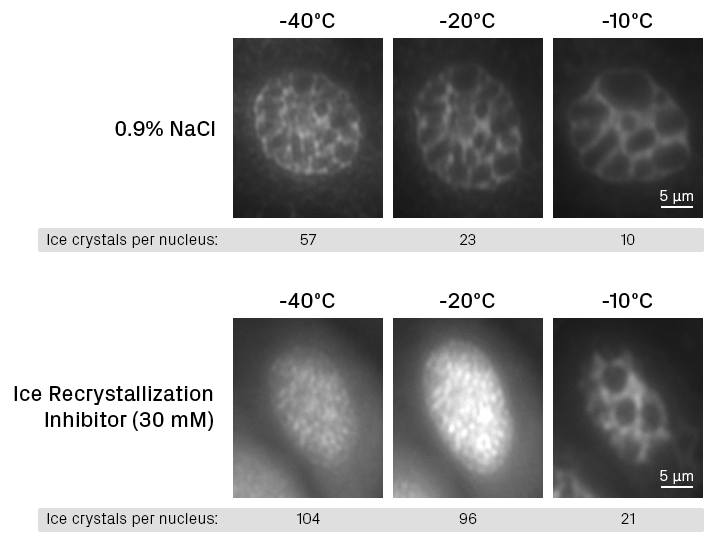
Another way is to put cryoprotective compounds into the samples to help protect against the damage that would accrue if they were transiently warmed. When developing ice recrystallization inhibitors, I was well aware of this. We have collected data sets that show that the ice recrystallization inhibitors keep the ice crystals small, and because of this, they’re able to protect the samples from temperature cycling, which occurs naturally in the handling of most cell therapy products.
What improvements are needed in the cold chain for cell therapies?
JA: The system needs to appreciate that maintaining temperature is critical to function. The manufacturers of cell therapies have to provide very detailed handling instructions as part of their Instructions for Use (IFU). Right now they don’t know what to put in that IFU. As a result, they can’t hold other parts of the cold chain accountable. They can’t instruct the clinical treatment centers how to handle those products any more than saying, “keep them cold and thaw them quickly,” which is really the essence of what’s in most IFUs.
We need to get better, and the only way to do that is with evidence and with the kinds of studies that we’ve been developing, but also building protections into the system. That’s where the ice recrystallization technology comes in. It provides a bit of a safety buffer to allow for those instances where adherence to an IFU may deviate.
Know what temperatures your products are seeing and understand what those profiles mean for your products because there is no, unfortunately, universal standard around — that is, your product can withstand X degrees of transient warming before it’s damaged. You have to do those measurements yourself because of the interplay between the cryoprotectant formulation and how those samples have been cryopreserved, which influences the structure of the ice and, as a result, how quickly they may be damaged from transient warming.
One example of technology designed to manage cold chain and reduce transient warming is the new CryoArc™ Pico.
What does the future of cryobiology look like?
JA: From a cell and gene therapy perspective, there will be improvements in cryoprotection. The PanTHERA ice recrystallization inhibitor technology, in my 25 years of working in this field, is groundbreaking. It solves some very fundamental challenges that the industry struggled with. Equally, Allison Hubel is working on her deep eutectic technology. Others are working on other stabilization technologies, such as hydrogels. There are a bunch of really neat technologies that are coming that may help deal with some of this as well.
We’re going to have tighter regulations around temperature control, for sure. Stability studies are going to be mandated by all regulatory agencies. You will need the stability data when you start to file for regulatory approval. This comes from the lessons learned from the first-generation CAR-T technology. The supply chain had challenges controlling temperature adequately, resulting in the loss of cell potency of the final product.
We’re already seeing molecular strategies to stabilize cells. How acceptable will those be to regulators? We’ll have to wait and see. But there are ways of genetically using CRISPR technology, for example, to upregulate certain stress response agents that would help the cell survive the cryopreservation process better.
We’re going to see organs cryopreserved in the next decade. I’m fairly confident of that. We’re already seeing partially frozen organs and the benefits of extended storage. I think we’re going to crack some of the challenges we’ve had with zebrafish embryos, granulocytes, and porcine sperm. Those are the three cell types that have never been successfully cryopreserved. Because of their physical structures, conventional cryopreservation strategies don’t work. Next-generation technologies are required to successfully cryopreserve these.
Learn More
To learn the latest developments in cryobiology, view Dr. Acker’s presentation “Impact of Transient Warming on Post Thaw Cell Functionality” and other talks from the inaugural Cryo Symposium for Cell & Gene Therapies.
About the Guest
Dr. Jason Acker

Dr. Jason Acker is the Senior Research Scientist with Canadian Blood Services and a Professor in the Department of Laboratory Medicine and Pathology at the University of Alberta, Edmonton, Canada. His cryobiology research program focuses on understanding the response of cells and tissues to ex vivo storage and the development of methods for their preservation and use as therapeutic products.